Triumphs Within the Turmoil
Last week, I used this space to consider lessons from the COVID-19 pandemic. While we have much work ahead of us, let’s acknowledge a few… Read More »Triumphs Within the Turmoil
What Have We Learned From the Pandemic?
We’re entering month eight of the COVID-19 pandemic, and although the response ― and impact ― has varied by country and even by state in… Read More »What Have We Learned From the Pandemic?
10 Minutes Lead to Lasting Mobility
Judi Gieske, a retired pediatrician, had just wrapped up a talk on vaccination and public health at a school in Ho Chi Minh City in… Read More »10 Minutes Lead to Lasting Mobility
Leading in the Era of COVID-19
Johns Hopkins Medicine is heading up the global fight against COVID-19 on multiple fronts. From testing to treatment, public health outreach to potential vaccines, experts… Read More »Leading in the Era of COVID-19
In-House Hub for Medical Education
Johns Hopkins Medicine and our affiliate Bermuda Hospitals Board (BHB) wanted to create a training hub that offers a comprehensive approach for medical education on… Read More »In-House Hub for Medical Education
Bolstering Bermudian Health
Johns Hopkins has been treating Bermudian patients and providing medical expertise on the island for more than 30 years. For the past year-and-a-half, our close… Read More »Bolstering Bermudian Health
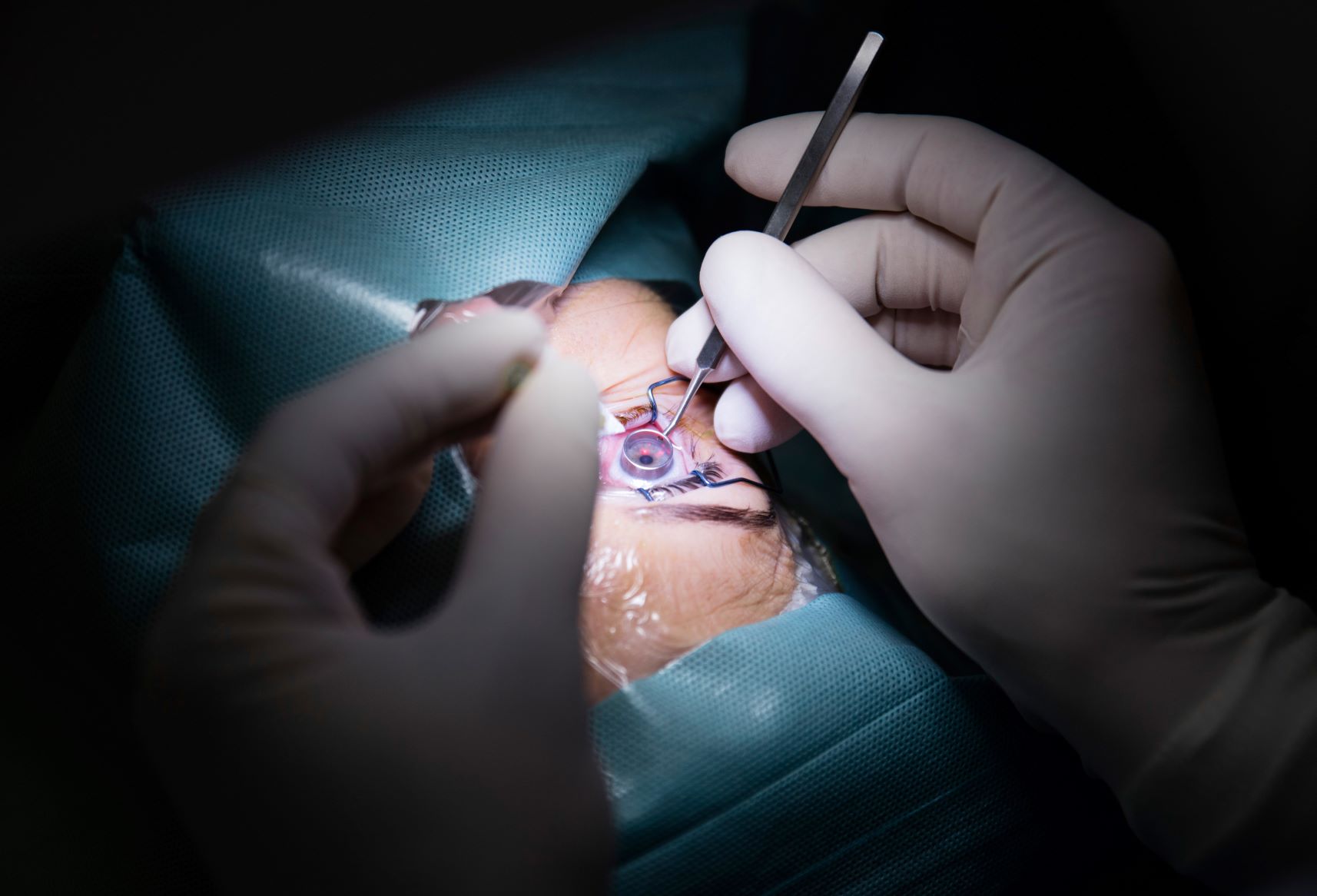
Banking on a New Supply
Cornea donations are much less common — perhaps less understood — than gifts of solid organs like the heart, kidneys and lungs. In fact, eye… Read More »Banking on a New Supply
Creating a Post-Stroke Roadmap to Recovery in Bermuda
When disease, trauma, congenital disorders or pain limit people’s physiological functions, rehabilitation helps them return to an active, independent life. For stroke patients, early and… Read More »Creating a Post-Stroke Roadmap to Recovery in Bermuda